Authors:
Okado, Jessica Baleiro 1 ; Avaca-Crusca, Juliana Sposto 1 ; Oliveira, Alexandre Lima 1,2 ; Gebieluca Dabul, Andrei Nicoli 1 ; Baratella da Cunha Camargo, Ilana Lopes 1,2
Abstract:
Objectives: Methicillin-resistant Staphylococcus aureus (MRSA) is a threat to the success of clinical treatment. Besides high antimicrobial resistance rates, the presence of heterogeneous vancomycin-intermediate S. aureus (hVISA) and heterogeneous daptomycin-non-susceptible S. aureus (hDNSSA) in the hospital environment is underestimated and is associated with treatment failure. The aim of this study was to investigate MRSA dissemination in a Brazilian hospital and to evaluate the efficacy of various treatment options in vitro.
Methods: MRSA strains were typed by MLST, PFGE and SCCmec typing. Minimum inhibitory concentrations (MICs) to daptomycin, linezolid, quinupristin/dalfopristin, teicoplanin, tetracycline, tigecycline, vancomycin and tedizolid were determined by broth microdilution. The presence of a heterogeneous population was detected by population analysis profile (PAP). Regarding hVISA and hDNSSA strains, the sequences and expression levels of genes involved in resistance to daptomycin and vancomycin were determined as well as cell wall thickness and autolysis.
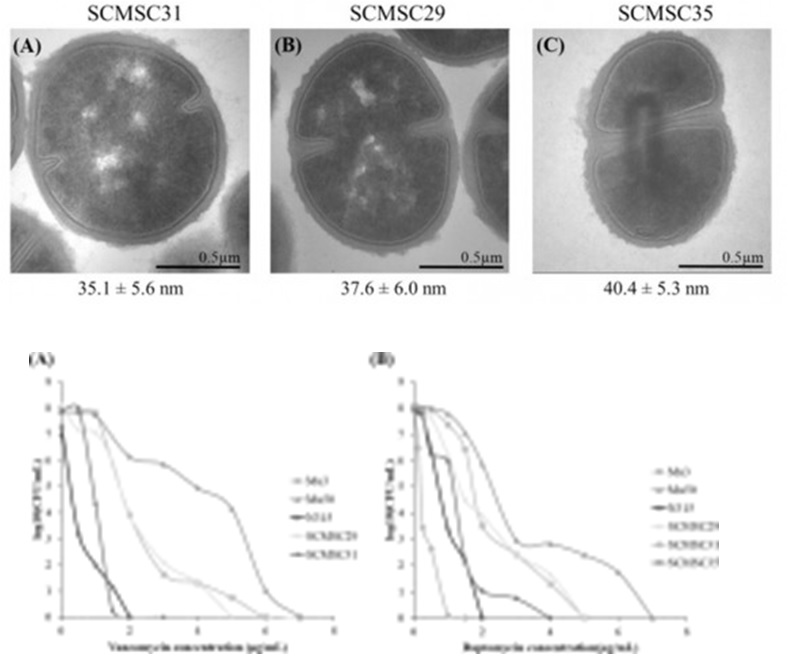
Results: ST5/ST105-SCCmecII lineage was prevalent amongst 27 clinical MRSA characterised in this study. Two hDNSSA strains (one also hVISA) were detected and were confirmed by PAP. Isolate SCMSC29 (hVISA and hDNSSA) showed increased expression of genes involved in cell wall metabolism, slight cell wall thickening, reduction of autolysis, and single nucleotide polymorphisms (SNPs) in the rpoB and mprF genes compared with the susceptible strain SCMSC31. SCMSC35 (hDNSSA) presented SNPs in the rpoB and mprF genes as well as a thickened cell wall.
Conclusions: Despite this worrying and hard to detect phenotype, treatment alternatives such as teicoplanin, linezolid, tetracycline, tigecycline, quinupristin/dalfopristin and tedizolid were all active against these isolates. (C) 2018 International Society for Chemotherapy of Infection and Cancer. Published by Elsevier Ltd. All rights reserved.
1 University of Sao Paulo, Sao Carlos Inst Phys, POB 369, BR-13569970 Sao Carlos, SP, Brazil
2 Federal University of Sao Carlos, Dept Evolutionary Genet & Mol Biol, Rodovia Washington Luiz Km 235, BR-13565905 Sao Carlos, SP, Brazil
Link to full article: https://www.sciencedirect.com/science/article/pii/S2213716518300857?via%3Dihub